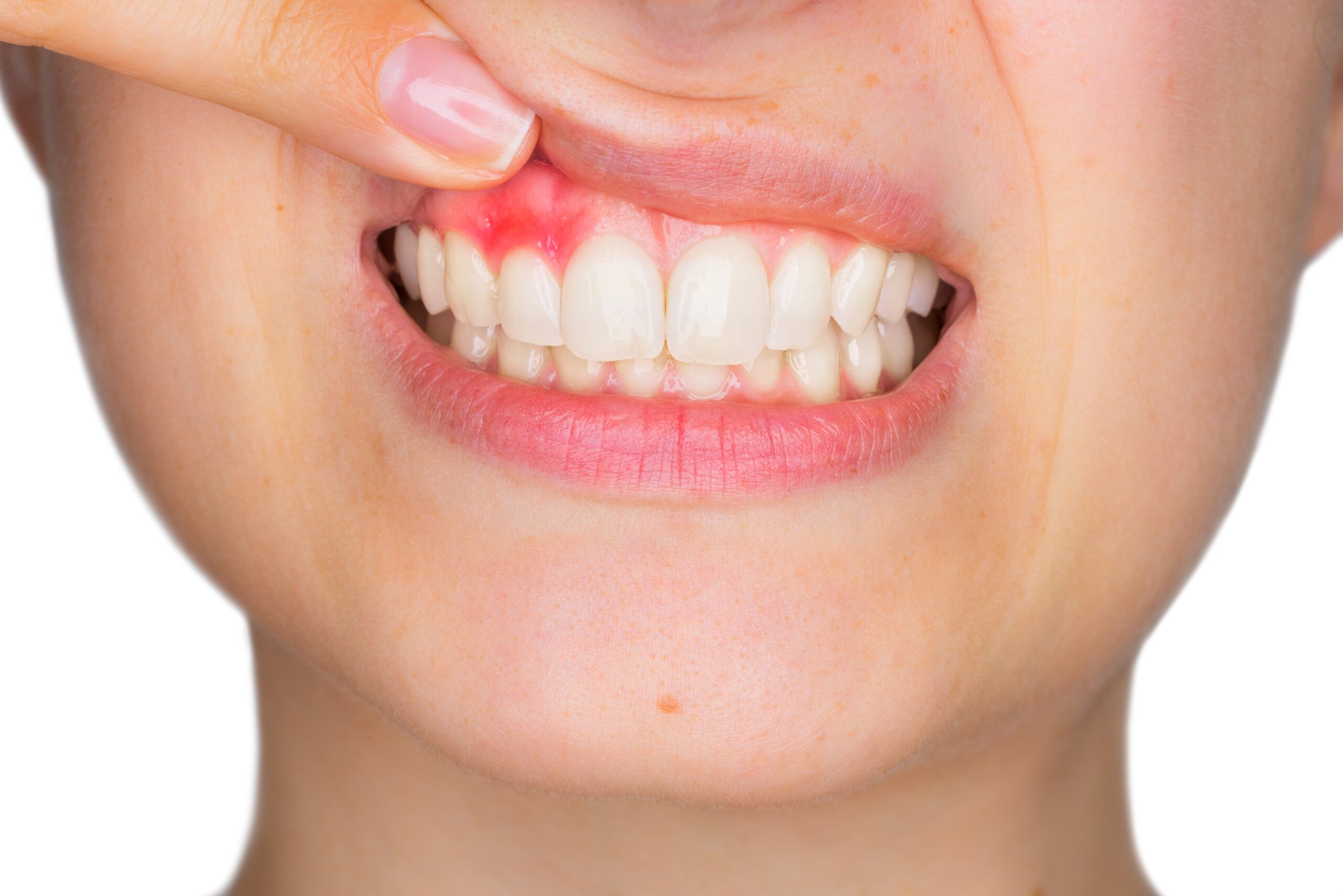
Peri-implantitis is a serious warning sign that your dental implant is in danger. It starts when plaque builds up around the implant. Then your gums swell, bleed, and pull away. Over time, the bone holding your implant begins to shrink. You may feel shame, fear, or anger. You invested money, time, and trust. Now you worry that the implant might fail. You also might feel afraid to eat, smile, or speak. A dentist in Los Angeles sees these injuries every day. The damage is silent at first. Then it can move fast. The good news is that you can slow or stop it with quick action. You need clear facts, not scare tactics. You also need a plan you can follow. This blog explains what peri-implantitis is, how to spot it early, and what treatment steps protect your implant.
What peri-implantitis means for your mouth
Peri-implantitis is gum disease around an implant. It attacks the soft gum and the hard bone. You cannot fix it with brushing alone. You need care from a trained team.
Here is what happens.
- Germs gather in sticky plaque around the implant
- Gums react and become red and sore
- A pocket forms between gum and implant
- Bone under the gum starts to melt away
Once the bone is gone, your body does not grow it back on its own. That loss can loosen the implant. Then chewing hurts. Your bite changes. Your face shape may change over time.
Warning signs you should never ignore
Peri-implantitis often stays quiet. You may feel no pain. You still get clear warning signs if you know what to watch for.
- Red, puffy, or shiny gum around the implant
- Bleeding when you brush or floss near the implant
- Bad taste or smell that will not go away
- Pus around the implant
- Gum pulling back and metal showing
- Implant crown that feels loose or moves
- New space between teeth near the implant
Any one of these signs is a strong reason to call your dentist today. Early care can save bone. Late care may mean you lose the implant.
Why some people face higher risk
Peri-implantitis does not mean you failed. It means your mouth needs help. Some risks come from daily habits. Other risks come from health history.
- Poor plaque control with brushing and flossing
- History of gum disease around natural teeth
- Smoking or vaping nicotine
- Uncontrolled diabetes
- Grinding or clenching teeth
- Implant placed in thin or weak bone
- Skipped checkups and cleanings
You can change some of these risks. You can stop smoking. You can control blood sugar with medical care. You can use a night guard. You cannot change the past. You can still protect the implant you have now.
How peri implantitis compares with gingivitis
Many people think all gum problems are the same. That idea causes harm. Gingivitis is milder. Peri-implantitis is more severe.
| Condition | Where it occurs | Main damage | Can it heal with home care |
|---|---|---|---|
| Gingivitis | Around natural teeth | Red, bleeding gums without bone loss | Often yes if you brush, floss, and get a cleaning |
| Peri implant mucositis | Around implants | Swollen gums without bone loss | Often yes with quick professional cleaning |
| Peri implantitis | Around implants | Gum swelling plus bone loss | No. Needs dental treatment and close follow-up |
You can read more on gum disease and implants from the National Institutes of Health at this overview.
How dentists find and measure the damage
Your dentist will use clear steps to check your implant.
- Ask about pain, bad taste, and bleeding
- Look at the color and shape of the gums
- Measure pocket depth with a thin probe
- Check for bleeding and pus from the pocket
- Take X-rays to see bone height around the implant
X-rays show if the bone is shrinking. Your dentist compares new images with old ones to see changes over time.
Treatment options that can protect your implant
Treatment depends on how far the problem has gone. You and your dentist can build a step-by-step plan.
- Professional cleaning around the implant to remove plaque and hard buildup
- Polishing or smoothing the implant surface so plaque sticks less
- Antimicrobial rinses or gels placed in the pocket
- Small gum surgery to lift the tissue and clean deeper
- Bone grafts to rebuild lost bone in selected cases
- Implant removal if bone loss is too severe
Early treatment is simpler and less costly. Late treatment can feel harsh. Quick action is an act of courage and self-care.
Daily steps that lower your risk
You can control plaque every day. These steps support your implant and your other teeth.
- Brush twice a day with a soft brush and fluoride paste
- Use floss or special implant threaders to clean under the crown
- Add an interdental brush sized for the space around your implant
- Use an alcohol free mouth rinse if your dentist suggests it
- Stop smoking and avoid all nicotine products
- Keep blood sugar in target range if you have diabetes
- Wear a night guard if you grind or clench
- Schedule regular checkups and cleanings
The Centers for Disease Control and Prevention shares more on gum disease and health at this gum disease page.
When to call your dentist right away
Do not wait and hope it will pass. Call your dentist soon if you notice any of these signs around an implant.
- Bleeding that happens often
- Swelling that lasts longer than two days
- New pain when you chew
- Pus or a pimple on the gum
- Loose feeling in the implant crown
Peri-implantitis can feel scary. You still have control. You can notice early signs. You can ask hard questions. You can follow a clear plan. Prompt care protects your implant, your smile, and your peace of mind.